
Why Weight Loss Comes Last: The Root-Cause Revolution…
Weight is not the cause—it's the consequence. If we focus only on the symptom, we miss the message.
We’ve been sold the idea that weight loss is a goal. In Functional Medicine, we see it differently: weight gain is a symptom—a visible signal that something deeper is out of balance.
Like the tip of an iceberg, excess weight often hides a vast landscape of hidden dysfunctions beneath the surface: insulin resistance, thyroid imbalance, chronic stress, inflammation, food sensitivities, toxicity, and hormonal dysregulation. Unless we address these root causes, weight loss will be temporary—or nearly impossible.
Let’s dive into what’s really happening beneath the surface.
The Iceberg Analogy: Why Weight Is a Symptom
As we discussed in our blog on goal setting, weight is rarely the root problem. It’s the effect. And when we focus on calories and workouts alone—without healing the systems underneath—we often hit a wall. Why? Because the body is not designed to lose weight. It’s designed to survive.
Instead of asking, “How can I lose weight?” the better question is:
“What is my body trying to tell me?”
In most cases the extra weight is just the tip of the iceberg where other underlying conditions may be hidden under the water. If these underlying conditions are not attended first, two things may happen:
It will sabotage weight loss progress
Sooner or later it will come up to the surface with more notorious symptoms. Hence, getting labeled with one of 55,000 diseases, syndromes, and illnesses from the ICD-11 Guidebook

7 Hidden Root Causes That Stall Weight Loss
1. Understanding Insulin Resistance: More Than Just Blood Sugar
According to the CDC, over 120 million Americans have insulin resistance or diabetes—and many don’t know it. Insulin resistance prevents cells from using glucose for energy, leaving excess sugar in the bloodstream and triggering fat storage.

Insulin resistance develops when excess glucose in the bloodstream makes it harder for cells to absorb and use sugar for energy. In response, the pancreas produces more insulin to maintain balance and keep cells fueled. While this compensatory increase in insulin can mask symptoms in the early stages, over time the system becomes strained.
As insulin resistance progresses, the pancreatic beta cells that produce insulin begin to wear out. Eventually, the pancreas can no longer produce enough insulin to overcome the resistance. This leads to chronically elevated blood sugar levels and, if left unaddressed, can result in prediabetes or type 2 diabetes.
What Causes Insulin Resistance?
Two of the most common contributors are:
A high-glycemic diet (rich in refined carbohydrates and sugars)
Chronic stress, which elevates cortisol and increases blood sugar production
These factors increase the glucose load on the body. When blood sugar spikes repeatedly over time, cells start to shut down their insulin receptors to protect themselves from overload—resulting in poor glucose uptake.
Ironically, people with insulin resistance often experience intense sugar cravings. This is because their cells are starved for fuel—even while blood sugar remains high—since glucose is circulating but not entering the cells efficiently.
Signs you may have it:
Sugar cravings
Fatigue after meals
Belly fat
A1C > 5.7% or fasting glucose > 95 mg/dL
What to do:
Eliminate added sugars, sweeteners, and white flours
Eat a protein-rich, healthy-fat breakfast
Avoid eating 2–3 hours before bed
Reduce stress (stress raises insulin!)
Consider testing: A1C and fasting glucose
📚 CDC Data on Diabetes & Prediabetes »
2. Thyroid Dysfunction: The Hidden Root of Fatigue, Weight Gain, and More
The American Thyroid Association estimates that about 20 million Americans have some form of thyroid disease—and up to 60% are unaware of their condition. Thyroid dysfunction can show up as underactivity (hypothyroidism) or overactivity (hyperthyroidism), and both can disrupt multiple systems in the body—often long before diagnosis.
How the Thyroid System Works
The thyroid gland, located at the base of the neck, plays a central role in regulating metabolism, energy, body temperature, digestion, and mood. To do this, it produces hormones using iodine:
T4 (thyroxine) – a mostly inactive storage hormone
T3 (triiodothyronine) – the active form that actually enters cells and powers metabolism
But here’s the key point:
The thyroid gland produces mostly T4. Only a small amount of T3 is made directly by the thyroid. The rest must be converted from T4 to T3 by other tissues—primarily the liver, gut, kidneys, and peripheral cells.
This conversion step is critical to feeling well—and it can be disrupted by things like stress, inflammation, nutrient deficiencies, and poor liver or gut health.
Hormone Regulation: The HPT Axis
Thyroid hormone production is tightly regulated by the hypothalamic-pituitary-thyroid (HPT) axis:
The hypothalamus (in the brain) releases TRH (thyrotropin-releasing hormone)
TRH tells the pituitary gland to release TSH (thyroid-stimulating hormone)
TSH signals the thyroid to produce T4 and a small amount of T3
This is a feedback loop, constantly adjusting based on your body’s needs:
🔻 If thyroid hormone levels drop → TRH and TSH rise → the thyroid ramps up hormone production
🔺 If thyroid hormone levels are high → TRH and TSH decrease → the thyroid slows down production
Why Thyroid Hormones Matter
Thyroid hormones affect every organ and cell in the body. They:
🔥 Regulate how fast you burn calories (metabolism)
❤️ Control heart rate and rhythm
🌡️ Set body temperature
🍽️ Influence how quickly food moves through the gut
💪 Regulate muscle function and strength
♻️ Control cell repair and regeneration
Even mild thyroid dysfunction can lead to fatigue, weight fluctuations, mood changes, digestive issues, and hormonal imbalance.
📚 Source: Michigan Medicine
Symptoms:
tiredness
being sensitive to cold
weight gain
constipation
depression
slow movements and thoughts
muscle aches and weakness
muscle cramps
dry and scaly skin
brittle hair and nails
loss of libido (sex drive)
irregular periods or heavy periods
Recommended labs:
TSH
Free T4, Free T3
Reverse T3
Thyroid antibodies (TPO, TG)
Actions to take:
These may vary depending on your lab results. Please follow your doctor’s recommendations. In some cases, you may need thyroid medication (e.g. radiated/ablated/removed thyroid).
Depending on the results, there are some lifestyle recommendations that we can suggest using Functional Medicine principles. If you want to know more please contact us.
📚 Thyroid.org – Thyroid Awareness »

3. Chronic Stress: The Hidden Hormonal Saboteur
Chronic stress is one of the most overlooked yet powerful disruptors of health and metabolism. It affects nearly every system in the body—and is often a major driver of stubborn, excessive weight.
What Happens When You're Stressed
Stress is your body’s built-in survival response to danger. When triggered, it shifts your system from the parasympathetic state (“rest and thrive”) into sympathetic mode—better known as “fight, flight, or freeze.”
In this survival state, your body deprioritizes functions like weight loss, digestion, fertility, and cellular repair. Instead, it activates a cascade of stress responses to keep you alive:
Raises blood pressure
Increases blood sugar for fast energy
Boosts cortisol and adrenaline levels
This is incredibly useful in short bursts—but chronic stress keeps your body stuck in overdrive, leading to metabolic dysfunction.

How Stress Blocks Weight Loss
When you're under stress, your adrenal glands release cortisol, a catabolic hormone that breaks down muscle tissue to produce glucose through gluconeogenesis. While this increases blood sugar temporarily, it also raises insulin resistance over time—making fat loss more difficult.
High cortisol also:
Suppresses thyroid function, increasing conversion of T4 to Reverse T3 (an inactive hormone that blocks metabolism)
Triggers sugar cravings
Promotes fat storage, especially around the abdomen
Even well-meaning habits like excessive exercise or over-restricting calories can backfire by spiking cortisol—which increases Reverse T3 and slows your metabolism.
On the other hand, prolonged stress or burnout can cause cortisol levels to drop too low, impairing cellular thyroid hormone uptake and leaving you feeling fatigued and stuck.
Common Sources of Chronic Stress
Stress doesn’t just come from your to-do list—it can be physical, mental, emotional, or environmental. Here are examples that may sabotage your weight loss efforts:
Emotional or spiritual distress
Ongoing trauma or grief
Chronic physical pain
Overtraining or high-intensity workouts without recovery
Low-calorie or restrictive diets
Poor sleep or sleep disorders
Overstimulation from caffeine, social media, or news
Hidden allergies or food/environmental sensitivities
Toxic exposures (mold, heavy metals, chemicals)
How to Know If You’re Chronically Stressed
You don’t always need a test to know your stress levels are too high. Some signs may include:
Sleep disruption or insomnia
Fatigue despite rest
Sugar cravings or emotional eating
Mood swings, anxiety, or irritability
Feeling “tired but wired”
Poor recovery from workouts
Brain fog or memory issues
We often override our own symptoms to keep up with busy lives. But your body keeps score—and it doesn’t lie.
👉 While cortisol testing isn’t always necessary, a 4-point cortisol panel (saliva or urine) can be helpful in certain cases to assess adrenal rhythm throughout the day.

Actions to Take
The best approach depends on the source of stress. You don't need to "do more"—you may need to do less and support your nervous system. These strategies can help:
Deep breathing or vagus nerve exercises
Meditation or guided visualization
Gentle yoga, walking, or stretching
Journaling or gratitude practice
Counseling, spiritual connection, or emotional release
Reducing stimulants (caffeine, screens, information overload)
📚 The Impact of Stress on Body Function »

4. Food Sensitivities: Inflammation from the Inside Out
“It’s not just about what you’re eating—it’s about what your body can tolerate, absorb, and process without triggering an immune response.” – Dr. Hyman
Food sensitivities are incredibly common, yet often missed. Unlike full-blown allergies, food sensitivities can fly under the radar for years because their symptoms are subtle, delayed, or show up in non-digestive ways—such as fatigue, headaches, joint pain, weight gain, or brain fog.
According to recent estimates, over 20% of people in industrialized countries have some form of food intolerance or sensitivity. The real problem? Most don’t know it.
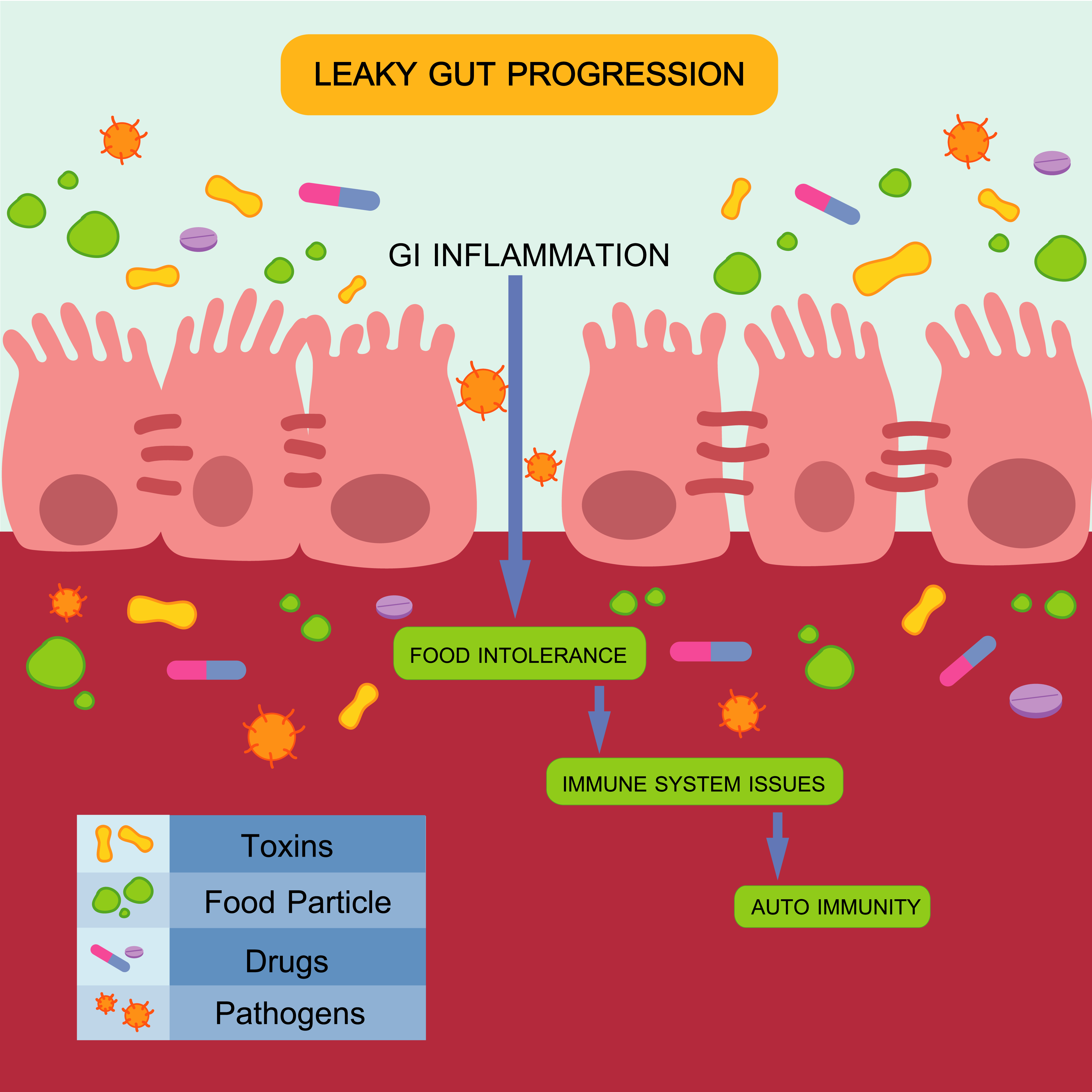
Why They Happen: Leaky Gut, Immune Confusion & Inflammation
Many food sensitivities begin with damage to the gut lining—a condition known as intestinal permeability, or what functional medicine calls “leaky gut.” When the gut lining is compromised, tiny food particles, toxins, or microbes can slip through and enter the bloodstream. The immune system sees them as foreign invaders and mounts a response.
Over time, this can cause chronic low-grade inflammation, which creates a vicious cycle:
Food sensitivities → Inflammation → Weight gain → More inflammation → More reactivity
This gut-immune interaction may be a hidden driver of stubborn weight gain, autoimmune flares, or even mood changes in people who “eat clean” but don’t feel well.
Common Food Sensitivities We See Often:
Dairy (even A1 casein-free versions)
Gluten
Corn and other grains
Soy
Nuts (especially peanuts, almonds, cashews)
Shellfish and seafood
Caffeine
Citrus
Note: You can react to healthy foods—especially if your gut lining is inflamed or your immune system is overloaded.
How to Know If You Have a Food Sensitivity
The gold standard is still an elimination and reintroduction protocol, like the one in my book UltraMetabolism. Here’s how it works:
Eliminate suspected foods for 21–30 days
Slowly reintroduce one food at a time every 2–3 days
Track symptoms (energy, digestion, mood, sleep, weight, skin)
Some people feel better within days—less bloating, fewer headaches, better sleep. Others feel worse upon reintroduction, which reveals what’s been silently inflaming them.
You can also explore lab-based options like IgG and IgA food sensitivity panels—but remember, no test is perfect. Your symptoms are often your best guide.

What to Do If You Have a Food Sensitivity
If a sensitivity is confirmed or strongly suspected, begin with a temporary, 100% elimination of the reactive food(s). This gives your immune system a break and your gut lining time to heal.
In many cases, sensitivities are not lifelong. Once inflammation is reduced and the gut is restored, you may be able to reintroduce the food in small amounts without issue.
To support healing, I often recommend gut-repair nutrients such as:
Slippery elm
Aloe vera
L-glutamine
Zinc carnosine
Targeted probiotics or immunoglobulins
Bottom Line
You can eat all the “right” foods, but if your body is reacting to them, you're still inflamed. Identifying and removing food sensitivities is one of the most powerful ways to:
Heal the gut
Lower inflammation
Balance immune function
Unlock weight loss naturally
This is one of the core pillars of functional medicine: remove the triggers, support the body’s healing, and let balance return.
📚 Food Intolerance – A Clinical Guide »
5. Toxins: The Hidden Obstacle to Healing and Metabolism
Most toxins are fat-soluble, meaning they get stored deep within our fat tissue—out of sight, but not out of mind. This includes heavy metals, pesticide residues, mold toxins, plastic chemicals, and pollutants in everyday beauty, cleaning, and household products.
When these toxins accumulate in the body, they disrupt your hormones, impair your metabolism, and stall healing—even if you’re “doing everything right.” In fact, toxins can make it difficult to lose weight or keep it off, because your body resists burning fat if doing so would release a flood of stored poisons into your bloodstream.
And here’s the catch: Some popular diet strategies like keto or intermittent fasting can actually mobilize toxins from fat tissue into circulation, creating an overload that does more harm than good—unless your detox systems are working properly.
How to Know If You Have a Toxin Overload
There’s no single test that can capture the full picture of toxic burden. Symptoms, history, and lifestyle exposures matter most. For example, if you have silver dental fillings, you’ve likely been exposed to mercury, a potent neurotoxin.
While some labs can test for heavy metals or mold toxins, these are only pieces of the puzzle. Functional medicine looks at the whole story.
Common signs of toxicity include:
Brain fog
Fatigue
Mood swings
Memory loss
Achy joints and muscles
Constipation
Poor appetite
Headaches
Confusion
Fine tremors
Actions to Take: How to Support Your Body’s Natural Detox Pathways
Before diving into detox protocols or major weight loss efforts, you must first unclog the detox pathways. Otherwise, you risk stirring up toxins without a way to safely excrete them.
Start here:
Hydration – Flush toxins through urine; aim for half your body weight (in pounds) in ounces of clean, filtered water daily.
Bowel Movements – You must be pooping at least once a day. Otherwise, toxins get reabsorbed.
Bile Flow – Healthy bile is essential for removing fat-soluble toxins. Bitters and nutrients like choline, taurine, or dandelion can help.
Sleep – Deep sleep clears out brain waste via the glymphatic system (a brain detox system most people have never heard of).
Toxin Avoidance – Go organic, especially with the Dirty Dozen. Ditch toxic personal care and cleaning products.
Once those basics are in place, you can consider supportive tools like:
Detox-supportive foods: Cruciferous veggies (broccoli, kale), garlic, cilantro, parsley, green tea.
Binders: Chlorella, activated charcoal, or bentonite clay (use under expert guidance).

When done right, detoxification isn’t a trendy juice cleanse—it’s a science-backed strategy to reclaim your energy, mental clarity, and hormonal balance. And it all starts with removing what’s harming you first.
📚 Adipose Tissue as a Site of Toxin Accumulation »
6. Sex Hormone Imbalance: How Environmental Factors Disrupt Your Hormones
Hormones don’t act in isolation. They function like a symphony—each one influencing the others. In women, an overload of estrogen is common and contributes to symptoms like PMS, weight gain, and fatigue. This is often due to impaired estrogen metabolism and clearance, or increased exposure to xenoestrogens—chemicals in plastics, personal care products, and conventional foods.
On the other hand, many women also struggle with high testosterone levels driven by insulin resistance, often seen in PCOS. In men, the reverse can happen: excess estrogen and low testosterone, which can stem from stress, environmental estrogens, and obesity.
Stress plays a central role. When the adrenal glands are constantly pumping out cortisol, testosterone production can drop. And with more body fat, adipose tissue itself acts as an endocrine organ—converting testosterone into estrogen.
How to Know If You Have a Hormone Imbalance
Common symptoms include:
Low libido
Infertility
Mood swings
Depression
Anxiety
Excess belly fat
Fatigue
Weight gain
Digestive issues
Hair loss or thinning
Skin and voice changes
Irregular periods
Lab testing can include:
Estrogen metabolites: estradiol, estrone, estriol
Progesterone metabolites: a- and b-pregnanediol
Androgens: testosterone, DHEAs, DHT
Actions to Support Hormone Balance
Limit BPAs and phthalates: Avoid plastic water bottles and containers
Limit parabens: Found in personal care items. Choose products without “-paraben” ingredients
Buy organic when possible: Especially for the "Dirty Dozen" produce
Be mindful with phytoestrogens: Found in soy, flax, legumes. They may support or hinder balance depending on individual needs

Hormone restoration may also involve addressing insulin resistance, managing stress, and in some cases, using hormone replacement therapy under medical supervision.
Supporting hormone health is not about chasing one hormone but understanding how the entire network works in harmony.
📚 Extra-Gonadal Estrogen Production »
7. Other Commonly Overlooked Root Causes
If you're eating well and exercising but still not losing weight, there's a good chance something deeper is going on. Weight loss is not just about "calories in, calories out." Your biology plays a bigger role than your willpower.
Let’s break down some hidden culprits that may be disrupting your metabolism and preventing your body from burning fat effectively:
🌙 Sleep deprivation: Skimping on sleep elevates your cortisol levels — your main stress hormone — which signals your body to hold onto fat, particularly around the belly. Poor sleep also disrupts appetite hormones like ghrelin and leptin, leading to cravings and overeating.
🏋️ Excessive exercise and calorie restriction: Contrary to what diet culture tells you, pushing your body too hard — especially with high-intensity workouts while drastically cutting calories — increases physiological stress. This keeps cortisol high and your thyroid sluggish, making your body resist weight loss.
🪑 Lack of movement (not just lack of workouts): Being sedentary — sitting most of the day — independently increases your risk of metabolic disease. Even if you're eating "clean" and exercising once a day, your metabolism suffers if you're inactive for long periods.
🥦 Micronutrient deficiencies: Your body can’t run on empty. Without adequate nutrients — especially B vitamins, magnesium, zinc, selenium, omega-3s, and protein — your metabolism, detox systems, and fat-burning machinery slow down. You can’t burn fat efficiently without giving your cells the raw materials they need.

“The key is to use a healthy, sustainable strategy for weight loss that balances your hormones and brain chemistry and doesn’t put you in a starvation response.” — Dr. Mark Hyman, The Blood Sugar Solution 10‑Day Detox Diet
Final Thoughts: Chase Health, Not the Scale
Skinny doesn’t equal healthy. And health isn’t a dress size.
We hope this information has been helpful and serves as a meaningful reminder: true health is about much more than a number on the scale or fitting into a specific aesthetic ideal. If we focus solely on weight or appearance, we risk neglecting the deeper markers of health—energy, resilience, hormonal balance, and long-term vitality.
Being thin, muscular, or "fit-looking" does not automatically equal health. While many individuals achieve body composition goals through consistent nutrition and movement, others resort to extreme measures—such as crash diets, unregulated supplements, stimulants, or risky procedures like steroid use or cosmetic surgery.
The truth is, thin people can still struggle with chronic inflammation, hormonal imbalances, digestive issues, autoimmune conditions, metabolic dysfunction, or cardiovascular disease. Health is not one-size-fits-all. When we chase external appearance without supporting our body’s internal function, we may fall prey to the cycle of fad diets, yo-yo weight loss, or unsustainable quick fixes like liposuction or bariatric surgery—which come with their own set of risks.
At Splendhealth, we are committed to shifting this narrative. Our priority is not perfection, but function. We help clients reconnect with their most valuable asset: their health—from the inside out.
The good news? Cultural norms are beginning to shift. Even as the U.S. weight loss industry exceeds $70 billion, the number of people turning away from diet culture is rising—thanks to movements centered around body respect, holistic health, and Functional Medicine.
